If your prescription is above -6.00 diopters, your eyes carry a risk most people never think about. The retina at the back of a highly myopic eye is stretched thin. That stretch creates weak spots. Those weak spots can tear. And here is the part that surprises most patients: you may feel nothing at all when it happens.
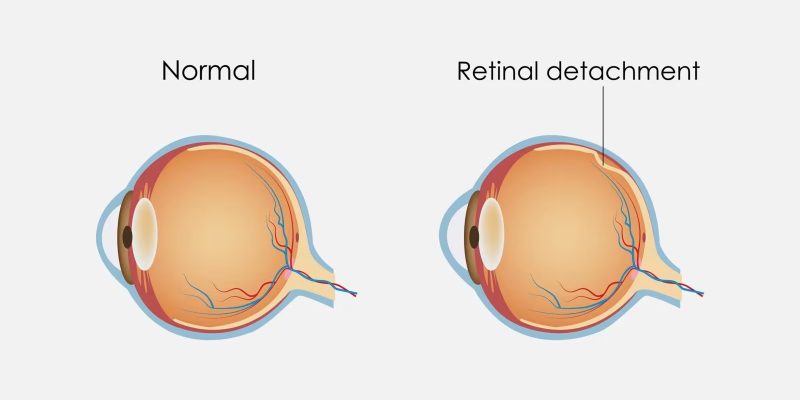
A retinal tear is not always painful. It does not announce itself. It simply occurs, and if fluid slips through the tear, a detachment follows. A detachment can cause permanent vision loss within days.
This is not a rare condition. Studies estimate that people with high myopia have a lifetime risk of retinal detachment up to 10 times higher than those with normal vision. Yet most highly myopic patients have never had a proper retinal exam. Many do not even know they need one.
What a Retina Exam Looks For
A standard eye exam checks your prescription and the general health of your eye. A retinal exam is a different appointment entirely. It goes deeper, literally and clinically.
The doctor begins by dilating your pupils with eye drops. This takes about 20 to 30 minutes to take full effect. Once dilated, the pupil opens wide enough to give the doctor a clear view all the way to the edges of your retina. That peripheral zone is exactly where high myopia does its damage.
The doctor uses a bright light and a specialized lens to examine the retinal surface in detail. They are looking for several specific findings.
The first is lattice degeneration. This is a thinning of the peripheral retina that creates a grid-like pattern of weak tissue. It is extremely common in high myopia. Many patients have it and never know because it causes no symptoms on its own.
The second is retinal holes. These are small breaks in the retinal tissue. They are different from tears, but both can allow fluid to pass underneath the retina.
The third is retinal tears themselves, which often occur at the edge of a lattice lesion. A tear is a more urgent finding than a hole.
The fourth is vitreous traction. The vitreous gel inside the eye can pull on the retina as it ages or shifts. In highly myopic eyes, this pulling is more likely to cause damage because the retina is already under tension from being stretched.
This level of examination requires subspecialty training. A general optometrist or ophthalmologist can dilate your eyes and spot obvious problems, but a retina specialist Las Vegas patients consult for high myopia cases has completed additional fellowship training focused entirely on the back of the eye. That difference in expertise directly affects what gets caught and what gets missed.
During one case I came across in research, a 29-year-old woman with -9.50 diopters went in for a routine glasses update. The optometrist noticed something during a basic exam and referred her for dilation. The retinal specialist found a horseshoe-shaped tear with early traction. She had felt nothing. No floaters. No flashes. She received laser treatment that same week and avoided what could have been a full detachment.
That story is not unusual. It is actually the most common version of how retinal tears in myopic patients are found. Accidentally. During an unrelated appointment. By a doctor who happened to look carefully.
This is why I believe every person with high myopia should have a dilated retinal exam at least once a year, not only when something feels wrong. The exam itself is straightforward. It is not painful. The dilation causes light sensitivity for a few hours. That is the biggest inconvenience. The information it provides is genuinely life-changing for your vision.
If you have been told your prescription is high and you have never had your peripheral retina examined, that gap in your care is worth closing now.
Symptoms You Should Never Ignore
Understanding symptoms is important, but I want to start this section with a caution. In high myopia, many retinal tears produce no symptoms at all. The ones that do produce symptoms are actually the more advanced cases. So the absence of symptoms does not mean the absence of a problem.
That said, there are warning signs that require immediate action.
The first is a sudden increase in floaters. Floaters are those small shapes, dots, or threads that drift across your vision. Most people with myopia have some floaters already. That baseline is normal. What is not normal is a sudden shower of new floaters appearing all at once. This can indicate that the vitreous gel has pulled away from the retina and torn it in the process. That event is called a posterior vitreous detachment, and it is a leading cause of retinal tears.
The second is flashes of light. These appear in the peripheral vision, often described as a lightning bolt or camera flash in the corner of the eye. They occur when the vitreous tugs on the retina. Occasional flashes can be benign. Persistent or frequent flashes alongside new floaters is a combination that needs same-day evaluation.
The third, and most urgent, is a shadow or curtain in your vision. This is not a floater. It is a fixed dark area, usually starting from one side or the bottom of your visual field, that does not move when you blink. This is the sign of an active retinal detachment. This is a medical emergency. You need to go to an emergency eye clinic or hospital eye department within hours. Not the next morning. Not after the weekend. The same day.
I spoke with a man named David who described his detachment experience. He noticed what he thought was a smudge on his glasses on a Thursday afternoon. He cleaned his glasses. The smudge was still there. He assumed he was tired. By Friday morning, the shadow had grown to cover the lower quarter of his vision. He went to urgent care, was transferred to a retinal surgeon, and had emergency surgery that evening. He recovered most of his vision, but not all of it. He told me directly: the hours he waited on Thursday were the hours that cost him.
That account stays with me. The window for treating a detachment before it affects central vision is narrow. Once the macula, which is the central part of the retina responsible for sharp detail, becomes involved in a detachment, the outcome is significantly worse even after successful surgery.
My honest opinion is that people underestimate eye symptoms. A floater feels trivial. A flash feels like a quirk. But in a highly myopic eye, these are biological signals worth taking seriously every single time.
Preventive Options: Monitoring vs. Laser
Once a retinal exam identifies a tear, a hole, or a high-risk lesion like lattice degeneration, the conversation turns to what to do about it. There are two main approaches, and the right choice depends on the specific finding and the individual patient.
The first option is monitoring. If a lesion is small, stable, and considered low risk by the examining doctor, watchful waiting is sometimes appropriate. This means scheduling follow-up exams every six to twelve months and returning immediately if any new symptoms develop. Monitoring is not a passive or careless choice. It is a clinically valid strategy for lesions that have a low probability of progressing to a tear or detachment. Some patients monitor stable lattice degeneration for years without incident.
The second option is laser photocoagulation. This is a procedure where a laser creates a series of tiny, controlled burns in a ring around the tear or weak area. Those burns heal into scar tissue, which effectively welds the retina to the underlying layer. The goal is to prevent fluid from passing through the tear and lifting the retina away. The procedure is done in an office setting, requires no incisions, and typically takes under 15 minutes. Patients usually drive themselves home, though some prefer not to because of the temporary effects of dilation.
The recovery is minimal. Some patients notice mild sensitivity or blurring for a day or two. The treated area may develop a small blind spot, but it is almost always in the far periphery and not noticeable in daily life.
I have a clear personal view on this. When a tear is identified in a highly myopic eye, I believe laser treatment is almost always the right call. The procedure is safe, quick, and effective. The alternative, waiting and hoping the tear does not progress, carries real risk. Retinal detachment surgery is far more complex, far more expensive, and far less certain in outcome than a 10-minute office laser procedure.
The argument for monitoring is strongest when the patient is highly engaged, attends every follow-up, and understands every symptom to watch for. In practice, life gets in the way. People miss appointments. Symptoms get dismissed. If a sealed tear cannot detach, that outcome is simply better than a monitored one that eventually does.
If you have high myopia, get the exam. If a tear is found, discuss laser seriously. The short-term inconvenience is nothing compared to what you are protecting.






Comments